Endeavor Physical Therapy
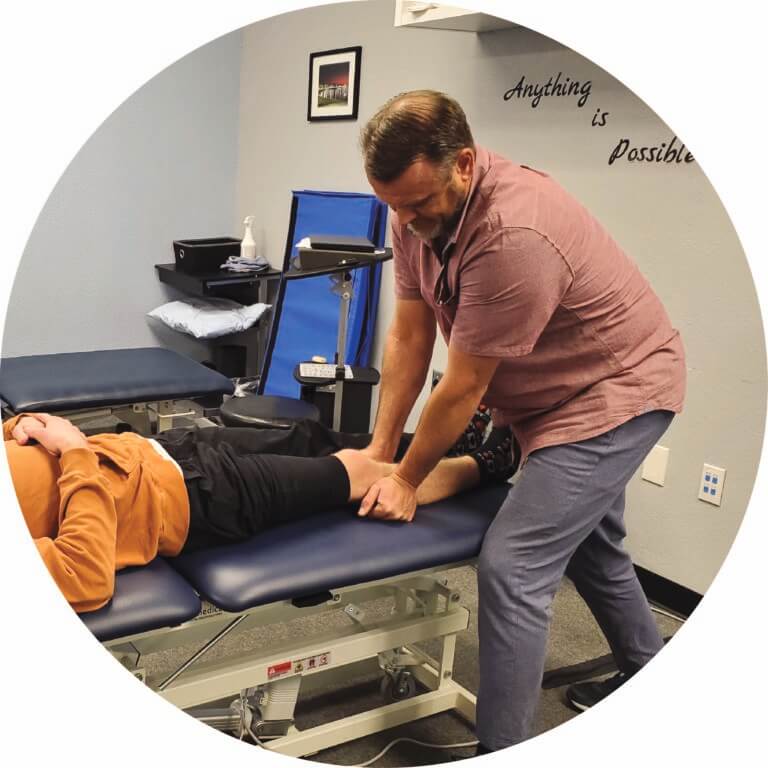
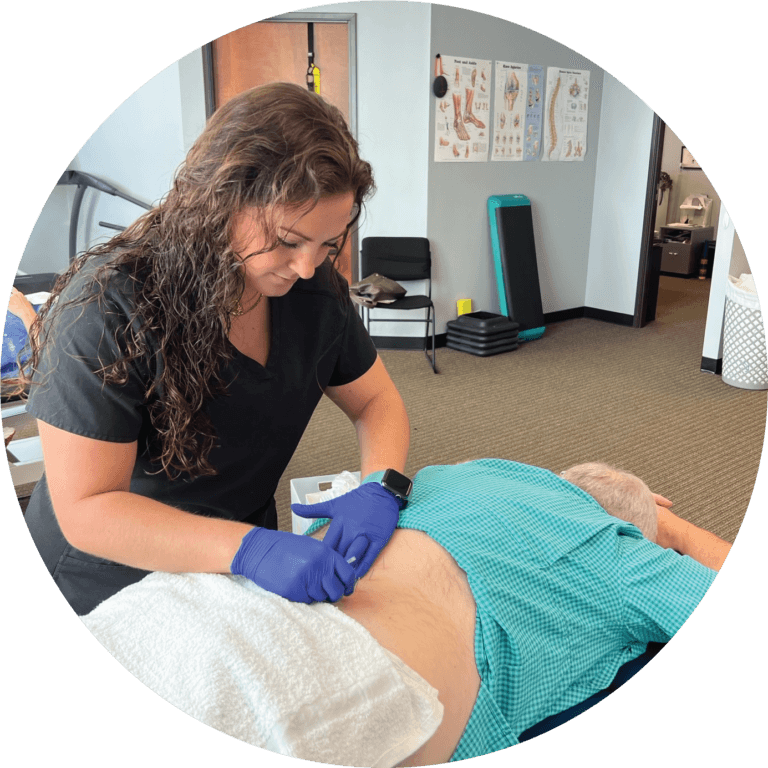
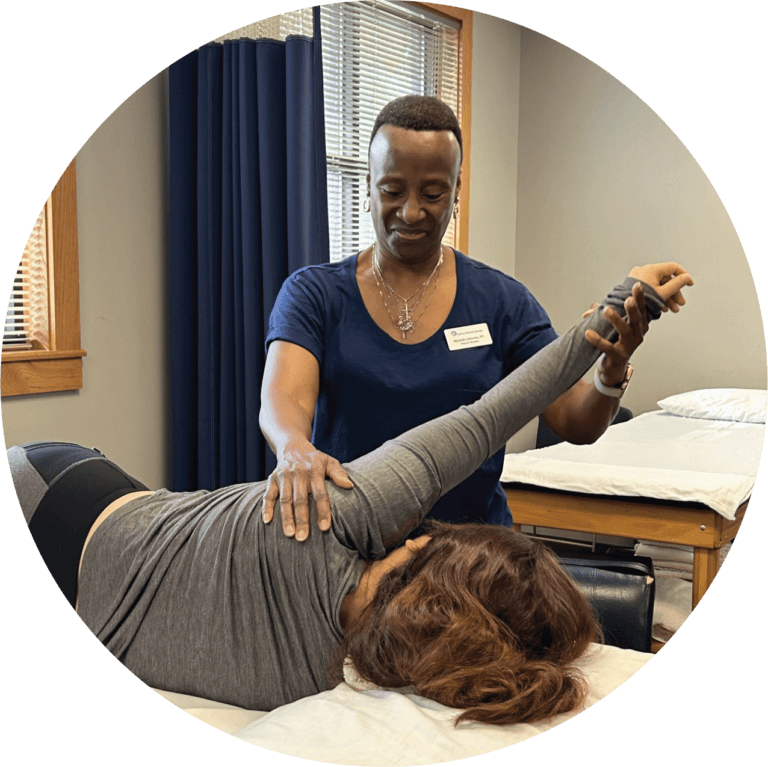
Endeavor Physical Therapy is an outpatient physical and hand therapy clinic that provides premier physical therapy intervention to patients suffering from musculoskeletal injuries pre-operatively or postoperatively. We provide treatment to the entire body system, from shoulders to the spine, hips, knees, elbows, hands, and ankles, and services for a wide range of musculoskeletal disorders and orthopedic injuries and conditions, specifically tailored for you.
From joint mobilization, therapeutic modalities such as dry needling, and functional exercise, our physical therapists provide both manual and non-manual therapy to target the problem and deliver custom-tailored rehabilitation programs that get real results. Our goal is to maximize your mobility, and function and improve your overall quality of life. As an owner-operated clinic, we are able to make our patients' needs our top priority.
Our Locations

South Austin
3809 S 2nd St
Suite D100
Austin, TX 78704
Southwest Austin
3100 W. Slaughter Ln
Suite 101
Austin, TX 78748

Northwest Austin, Four Points
6911 Ranch Road 620 North
Suite B-200
Austin, TX 78732

North Central Austin
1033 La Posada Drive
Suite 230
Austin, TX 78752

Anderson Lane
3202 W. Anderson Lane
Suite 202
Austin, Texas 78757

Hutto
210 Ed Schmidt Hwy
Suite 250
Hutto, TX 78634

Domain
12001 N. Burnet Rd
Suite G
Austin, TX 78758
Cedar Park
1120 Cottonwood Creek Trail
Bldg B, Ste 220
Cedar Park, TX 78613

Kyle
920 Kohlers Crossing
Bldg E, Ste 550
Kyle, TX 78640

Manor
11300 Hwy 290 E
Bldg 1, Ste 140
Manor, TX 78653

Pflugerville
1601 E. Pflugerville Parkway
Bldg 1, Ste 1202
Pflugerville, TX 78660

San Marcos
151 Stagecoach Trail
Suite 103
San Marcos, TX 78666

Round Rock East
896 Summit St.
Suite 102
Austin, TX 78664
Round Rock West
16020 Park Valley Dr.
Austin, TX 78681
Bee Cave
3944 Ranch Road 620 S
Bldg 8, Ste 203
Bee Cave, TX 78738

Waco
1200 Richland Dr Ste G
Waco, TX 76710
(formerly Bosque River Physical Therapy)
Sun City
4847 Williams Dr
Suite 103
Georgetown, TX 78633

Georgetown Physical Therapy
3415 Williams Drive
Suite 145
Georgetown, TX 78628
Services





































